Many GP practices in Scotland do not have enough clinicians to meet the needs of their patients, creating a capacity/demand imbalance that is resulting in a general practice sustainability crisis. GPs in Scotland report that having an unmanageable workload is the number one problem in their working lives. This is impacting the wellbeing of GPs and is causing their teams a great deal of stress. It is also harming the experience that patients have with their practice and the level of access to care they can receive. It will undoubtedly impact negatively on the health outcomes of patients.
The purpose of this guidance is to support GPs and their practices in these difficult circumstances to safely manage their workload to a reasonable level. It can also be used as a guide by all practices to assess whether their level of service provision and patient access is consistent with the BMA's recommendations. It is hoped that this guidance will help practices to establish a reasonable and safe workload – to protect GPs, their staff, and patients – and ultimately help maintain GP services in the long term.
It should also be applicable to practices with a PMS/Section 17C contract, except that those contracts are negotiated locally between a practice and health board which will contain specific contract variations. Practices with a PMS/Section 17C contract will want to carefully check their contracts before following our advice.
Safe workload advice
Until there is better support and funding to reverse the sustainability crisis, GP practices must be prepared for increasingly difficult circumstances and further workload challenges. Many practices will need to protect themselves and their patients from the unsafe consequences of excessive workload.
In many practices the workload crisis is so severe that we recommend practices take urgent action to preserve patient care and their own wellbeing. Practices will need to decide how to prioritise care and day-to-day activity accordingly. These actions will inevitably result in some patients waiting longer, or issues that do not need to or cannot be dealt with in general practice being directed elsewhere.
GPs are reminded that HBs (health boards) are ultimately responsible for the provision of primary medical services for patients. While HBs contract with GP practices to deliver this responsibility, GP practices are not a safeguard for all NHS services or providers of last resort – and they cannot be expected to operate beyond the terms of their contract or undertake a workload that is unsafe.
Key guidance for GP practices with excessive workload
1. GP practices can limit their workload and direct patients to other NHS services
GP practices can limit their workload, consistent with the advice that follows, to protect themselves, their staff, and patients. It is acceptable for GP practices, where they have reached their safe working limit, to direct patients to other HB (health board) services. If other HB services are unable to see patients – that is not the responsibility of the GP practice.
Practices can direct emergency and urgent problems to other health board services including NHS 24 (111), accident and emergency, and the Scottish Ambulance Service.
Practices usually start the working day with capacity to deal with new problems, however if demand is higher than expected some practices may reach a stage where they consider that they have reached their safe maximum activity for that day. If they determine that taking on more clinical activity is a greater risk they may decide that the safest option is to divert their telephones to answer machine with the following message, which is approved by the BMA.
BMA approved message to patients where safe practice capacity has been exhausted:
"The practice is currently experiencing unmanageable demand for urgent care. Taking account of our practice team’s safety and the availability of other options for patient care we are not able to manage any more patients today. We are sorry for this inconvenience, which is beyond our control. If you have an urgent medical problem that you believe cannot wait, then you should seek help from other NHS agencies including NHS24 on 111 or through accident and emergency."
We do not advise practices substitute this message with a text message to all patients – this message is intended for patients phoning the practice only.
It is unknown how often the call diversion action will be necessary for practices, but it is hoped that these are exceptional circumstances and will be rare – we advise any practice who takes this action to notify their HB (health board) so that they can better monitor the pressures in general practice and can look to offer additional assistance to that practice going forward to avoid the need for the action to occur again. Your local medical committee (LMC) can provide details of the most appropriate health board contact.
In Lothian, the LMC and Health Board were able to jointly agree the following version of this message, giving practices greater confidence to use it:
“For any life-threatening emergencies please attend A+E or call 999. The practice is under significant pressure due to demand for appointments. This demand has now far outstripped our safe working levels. If you require urgent attention please hold and your details will be taken by one of our admin team (or complete an econsult request online). Our on-call doctor will triage all urgent requests. They will manage as many cases as they can in order of clinical need. However, it may be that they cannot attend to your needs today. If you have not heard back from the practice by 6pm and you feel you cannot wait until tomorrow, then please look at the symptom guides at www.nhsinform.scot or call 111 for advice."
An alternative to diverting to an answering message is for reception staff to inform patients that a safe capacity has been reached, the practice is unlikely to be able to see them, and if they do not hear back from the practice before the end of practice opening hours (and their condition cannot wait) to contact NHS 24. Practices will want to choose a system that will work best for their own circumstances and ways of working.
2. A safe level of working for all GPs is up to 25 patient contacts per day.
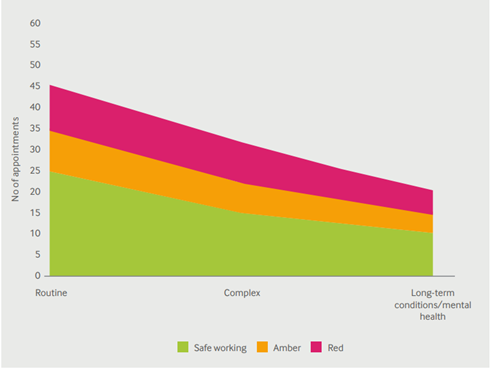 Safe working in general practice (BMA 2018)
Safe working in general practice (BMA 2018)
The number of safe patient contacts reduces as complexity of the contact increases. Our advice on a safe number of appointments was published in 2018. We expect that 25 patient contacts per day includes a mix of face-to-face and remote contacts. We believe the complexity of patient contacts is generally increasing and resulting in more non-patient facing clinical tasks.
3. Safe working levels should apply to duty doctors
Many practices in Scotland operate with a duty doctor arrangement that picks up urgent and unscheduled care. This can be efficient - allowing the GPs to focus on planned care delivery - but also risks uncontrolled and excessive workload which is not consistent with safe working landing on the duty doctor. As detailed above, it is important to have a policy for diverting urgent care needs where they cannot be met safely by the practice.
We are aware this could be difficult to implement for all practices, but innovative approaches have allowed practices across Scotland to protect all GPs from unsafe workload demands.
Practices need to be aware that there is no requirement under the GMS contract for GP practices to have a duty doctor and we are increasingly concerned that duty doctors are working beyond the levels recommended in this guidance.
Successfully applying this guidance means that duty doctors cannot and should not act as a sponge to soak up demand from patients who are finding access to the practice slower than desired. Where practices choose to operate a duty doctor system, they should consider having clear policies for the type of contacts that is appropriate to be passed to a duty doctor. Practices may also wish to consider indicating to patients that a message about their call will be passed to the duty doctor to consider, but that the duty doctor will only call back where it is clinically urgent and there is sufficient capacity in the practice to allow them to do so, rather than creating an automatic expectation of a duty doctor consultation.
4. GP practices can book 15-minute patient appointments
We strongly recommend practices take immediate measures to move to 15-minute appointments. This will not mean 15 minutes with the patient, as non-patient facing time will always be required for documentation and other tasks to complete the care episode. Without increasing the total time spent on consulting in a day, GPs can preserve quality of care, by moving to 15 minute appointments.
We recommend that no more than three hours per session is spent in consultation with patients to allow adequate time for administrative work/tasks. Within these limits, adequate rest breaks must be taken. Extending sessions beyond this time risks harm to patient and clinician. Increasing appointment length to 15 minutes would mean a reduction in the absolute number of appointments per session to safe levels for clinician and patient.
Controlling your workload under the contract
In addition to the measures above on limiting patient contacts, directing to other NHS/HB services, and extending appointments to 15-minutes there are several options that practices can use under the contract to help protect themselves from unmanageable workloads. While no single option is likely to be a full solution, it may be possible through a variety of measures to reduce the workload of a practice to a level that is hopefully safe and manageable in the longer term.
If your practice workload is unmanageable, you may wish to consider the following:
1. Inform the relevant health board and consider local escalation processes
Let the health board know that workload at your practice is regularly reaching an unmanageable/unsafe level which is impacting your ability to provide safe care for your patients.
Formally write/email to the health board informing them that your practice workload is unmanageable and that you are seeking the health board’s support to resolve the problem. Health boards are ultimately responsible for primary care and have a responsibility to support practices.
When writing to the health board, communicate the reasons why the practice workload is unmanageable. Reasons may include (but are not limited to):
- the patient list being too high
- unfilled vacancies/inability to recruit GPs or other practice staff
- inadequate or unreliable HB services to patients
- inadequate space to accommodate the practice responsibilities
- insufficient financial resource, etc.
You will also want to highlight any practical help the health board could provide to improve the situation. Practices will want to consider the health board’s reply and any suggestions that might improve your workload. If the health board does not respond promptly or you do not consider their response helpful, you should consider implementing other aspects of this advice as deemed necessary by the practice.
You may also wish to inform your local medical committee (LMC) of your practice workload difficulties. LMCs are helpful in highlighting any local support or systems in place that could help your practice. In some health board areas, local escalation processes are in place that allow practices to reduce their services to patients if faced with serious capacity challenges.
2. Consider reviewing practice arrangements for patient access
GP contractors are required to carry out their obligations under the contract with reasonable skill and care and to provide for their patients’ reasonable needs. Practices must exercise their professional judgement in allocating their resources in accordance with their usual ways of working. This applies to the processes the practice puts in place to allow patients to access the services they provide. Practices should regularly review their access arrangements to ensure the best for patients within their practice capacity.
GP practice capacity is finite. If demand exceeds capacity, then practices may prioritise care for those patients with the greatest need. Unfortunately, not every patient can be seen when they wish. It is reasonable for GP practices with unmanageable workloads to limit either the number of appointments/ contacts they have or to increase appointment length.
Secondary care prioritise patients on waiting lists based on clinical need. In the absence of sufficient capacity, general practice can prioritise access based on clinical need to allow GPs to focus their resources on those with the greatest and most urgent need. This may mean some patients waiting longer for an appointment with their GP and being booked into available advance appointments weeks ahead or alternatively, they may consider directing the patient to another health board service. The practice can limit the number of weeks ahead that appointments can be booked based on organisational need and taking account of managing the risk that a patient’s condition may deteriorate whilst awaiting their appointment. Practices should advise patients booked into advance appointments to call the practice again if their condition deteriorates.
3. Pushing back on inappropriate workload
We provide template letters to support GP practices in pushing back on inappropriate work from secondary care and health boards. Practices may use these templates where they consider that requested work is inappropriate. LMCs (local medical committees) and the BMA can help practices determine if work they are being asked to do is inappropriate.
4. Managing patient complaints
Patient complaints can be a significant source of anxiety and stress for GPs, particularly when they occur despite GPs going above and beyond to care for their patients in the face of workload challenges. Practices may worry that implementing safe working limits could lead to their practice receiving more complaints from patients who are frustrated at the level of access to appointments that the practice is able to provide.
It is important, however, to recognise that the amount of capacity that practices have available and the number of appointments they can safely offer is ultimately driven by Scottish Government’s investment and workforce planning decisions and the level to which it wishes to prioritise General Practice. While practices have flexibility in how they deliver their services, they do not control the overall funding envelope that can be used to deliver GP services or have responsibility for ensuring sufficient new GPs are trained and existing GPs are incentivised to remain in practice.
Complaints about access to appointments are often complaints indirectly about Government policy. While practices must treat all complaints seriously, they can and should highlight this fact to patients and may wish to suggest patients contact their MSP or the Scottish Government to make clear that general practice needs greater resourcing to be able to provide more appointments.
Practices should also recognise that the risk of more serious complaints relating to standards of patient care falling short of what a patient expects are more likely to occur when clinicians are working beyond capacity and at increased risk of making mistakes. Implementing safe limits on workload can help reduce the chances of such mistakes occurring and serious complaints being subsequently received.
5. Consider formal practice list closure
Practices can notify the health board that they wish to close their patient list to achieve a more manageable and safer workload. There is BMA guidance for practices in Scotland considering closing their list. Practices wishing to close their list will need to send a ‘closure notice’ to the health board. Following receipt of such a request, the health board will have 28 days to enter discussions with the practice to resolve the practice’s concerns. This will include discussing what support the health board can give to enable the practice to keep its list open. Practices will want to consider our advice above on safe working to determine a reasonable list size that would trigger the reopening of the list. Health boards can reject applications by practices to close their list following consideration by an assessment panel. This decision can be challenged via an appeal to Scottish Ministers. It is important to note that patients can only be allocated to practices with a closed list by the health board when most or all practices in a board area have a closed list.
6. Consider reducing your practice area
Practices can write to their health board requesting to reduce their practice area. This can help control the size of the practice list and limit travel for home visits. The health board’s decision process for such requests is similar to the process for requesting formal list closure. Once a notification has been received, the health board must enter discussion with the practice to resolve the matter within one month. Discussions must be concluded within three months of having received the notification.
7. Consider reducing service provision of additional or enhanced services to maintain core services
Practices are not obligated under the 2018 contract to provide additional or enhanced services (local, national, or directed). Practices that wish to cease additional services can opt out under the contract or serve notice to the health board if they wish to cease enhanced services. This will impact practice funding.
Through negotiations with Scottish Government, BMA Scotland has progressively moved historical funding from ‘non-core’ elements like QOF and vaccinations to the global sum and the income and expenses guarantee. Practices should consider whether it is protective and/or cost effective to continue providing additional or enhanced services.

