Being deafblind would be more than enough to contend with as a trainee doctor, let alone all the doubters and discrimination.
Yet, Alexandra Adams wrestles with other physical challenges too. During the pandemic, these conspired to put her in hospital for 17 months and brought her studies to a screeching halt.
Now, after a two-year interruption, she is back at medical school in Cardiff, doing clinical placements at a hospital where she was a long-term patient, fighting off the flashbacks.
Even now that her health has stabilised, she is on 24-hour oxygen, has a gastrostomy tube and drain, and is sick many times a day. She is also highly prone to joint dislocation and has had sepsis seven times in one year. ‘My life is definitely not boring,’ she says.
In it all, Alexandra’s determined to stay positive. Unexpectedly, she found herself thrust back into the role of diversity advocate recently after she introduced herself to TikTok as a deafblind medical student and went viral.
But she is still coming to terms with what’s happened in the past two years.
23 ICU visits

Alexandra would like to be able to trot out unreserved truisms about her experiences as a patient preparing her to be a better doctor. They have, of course, but it is not quite as straightforward as that.
The truth is that the 17 months she spent in three different hospitals, during the COVID pandemic, left her traumatised – and doubting her choice of career.
‘It is something that I thought about every day as a patient,’ she says. ‘At one minute, I’d be feeling I’m learning so much about medicine and how to treat my future patients. But the next, I wanted to run as far away from medicine as possible.’
The respiratory and digestive issues she has had since her mid-teens had been growing progressively worse. Respiratory muscle weakness has landed her in ICU 23 times.
During the first lockdown and her fourth year at medical school, her condition had deteriorated so far that she was admitted to ICU three times. On the day of her first discharge, her rental agreement was terminated with immediate effect on the grounds that her health and hospital visits were ‘putting other tenants at risk’.
When Alexandra was admitted in July 2020, just after her parents had managed to find her new accommodation, she was severely malnourished, fitting and fighting to breathe. This time she stayed in.
‘My fault’
It took three months in hospital for her to be diagnosed with Ehlers-Danlos syndrome, a rare genetic condition resulting in faulty connective tissue. In Alexandra’s case, this has affected her immune, cardiovascular, respiratory and gastrointestinal systems, causing, among other things, intestinal failure and gastroparesis (delayed gastric emptying and stomach paralysis). She also has extreme joint hypermobility.
Then, on Boxing Day, she tested positive for COVID. ‘The hospital was drowning in COVID by then: pretty much every ward became a red ward. I was in gastroenterology when I caught COVID. The patient next to me basically said it was my fault and “now you’re going to spread it to the rest of us”.’
In fact, the three other patients on her bay all caught COVID; Alexandra was the only one who survived, after a month in the red zone. ‘I knew it wasn’t my fault, but I felt really guilty that the three others didn’t make it. It destroyed me.’
In early March 2021, she was transferred to a hospital in London for six months, then after a brief respite at home in Kent, she was back in hospital in Wales. For much of the time, Alexandra was very unwell, strongly medicated, bedbound, unable even to lift her head. COVID meant she couldn’t have visitors for many months; playing the piano in the hospital chapel, when she grew stronger, was her only respite.
‘There were nights when I was bawling my eyes out and thinking: I don’t have a future, I don’t have a purpose. I didn’t want to be here any more.’
What kept me going was a voice reminding me: ‘This is one hell of a journey but it’s all lived experience you’re going to learn from.’
‘It’s going to be valuable, whether it’s through being able to help people, making you resilient, or making you more grateful for the little things”.’
Contrasting care experiences
Some of the care she received, especially from nurses at St George’s Hospital in London, was first-rate. Nurses in Wales brought her ICU bed outside so she could meet Winnie, the new family Cavapoo puppy.
But some experiences she found deeply distressing. What she saw on the COVID ward was ‘horrific’, though beyond anyone’s control.
 Alexandra: ‘I’m just trying to focus on the good stuff’
Alexandra: ‘I’m just trying to focus on the good stuff’
But she has found it harder to come to terms with what she feels was unkindness and neglect from some.
Alexandra knows staff everywhere were – and remain – under extreme pressure. But she felt some expected her to ‘just get on with it’ and deal with things better because she was a medical student.
Before she was diagnosed with the rare condition Ehlers-Danlos syndrome, she felt medical staff believed her condition was ‘all in her head’. Frequently afterwards, she was made to feel a nuisance – even when she was in excruciating pain or genuine distress.

At one point, when she had a painfully infected central line site, which turned out to be severe sepsis, she was told: ‘Your neck’s not fractured! Move it!’
And when she asked about the long-term prognosis for people with Ehlers-Danlos, scared for her future, a doctor replied, ‘You’re a medical student: surely you’re competent enough to work it out for yourself.’
‘The doctors were in a very difficult position because I was a complex case and nothing seemed to be working but I did get a lot of sarcastic comments,’ she says.
Months after requesting mental health support, she saw a psychologist who offered only dietary advice and suggested she try kefir. And the promised discharge letter to her GP and referral to a specialist hospital never materialised. She now has a drainage tube in the wrong place and no overseeing consultant.
‘As a patient I feel I’ve slipped through the net – but as a medical student I still love the NHS and couldn’t think of a better place to work.’
Financial pressures
Towards the end of last year, Alexandra decided to ignore her health challenges and resume her studies. She says she had ‘reached a point where I felt nobody cared for me’ so she stopped caring for herself. She was passed fit to return in January and began catch-up placements in June, with a view to restarting her fourth year in September. Her previous year group has since graduated.
There are other pressures. She’s not sure how she can fully fund her accommodation. Her requirements are specific: her blindness and chronic fatigue mean that she can’t live too far from the university, so rooms tend to be more expensive.

The extra equipment and tech she needs are costly too. Her parents can’t afford to help: the whole family has been hit hard emotionally, physically and financially by events of the past two years.
In 2020, Alexandra took the ‘uncomfortable’ step of crowdfunding for her accommodation and was able to fund a two-year rental contract. Unfortunately, she was in hospital for much of that time.
To help with her finances, she’s taken on bank work as a phlebotomist at the same hospital where she was admitted as a patient in July 2020.
‘I took a little detour after my shift the other day and went into the chapel to play the piano again. I cried because I saw the old me in the distance, a patient in a gown and a wheelchair. But I just have to get over that.’
Alexandra has set herself an 870-mile sponsored walking challenge this year to raise money on GoFundMe for pianos in NHS hospitals.
Social media star
In public and on social media Alexandra is resolutely cheerful. Unexpectedly, she has attracted the attention of a new audience by posting a short video on TikTok about returning to medical school as a ‘deafblind medic’. It triggered a familiar storm of disbelief and trolling: some impressed by her resolve, others ridiculing her ambition.
‘It was proof that ableism is very much still out there,’ she says. ‘But people were asking some genuine questions too, such as: How would you take blood if you can’t see or how would you hear someone’s heart?’ Alexandra has been deaf from birth; she has no sight in one eye and only 5 per cent in the other.
She started making videos addressing these questions, explaining, for example, how her stethoscope links by Bluetooth to her hearing aids, how she accesses veins by touch or uses magnification to read scans. The first TikTok went viral, with 2.4 million views and counting.
I do believe you don’t need the best vision or hearing to be a good doctor: having insight and empathy is the most important thing.
‘But wait till I tell TikTok I stick needles into people as a phlebotomist. That’ll really tee some people off!’
Diversity advocate
This major setback is not Alexandra’s first. In her early teens she was part of the GB Paralympic swimming team, training for the London 2012 games. But complications following stomach surgery left her in hospital for a year and ended her swimming career.
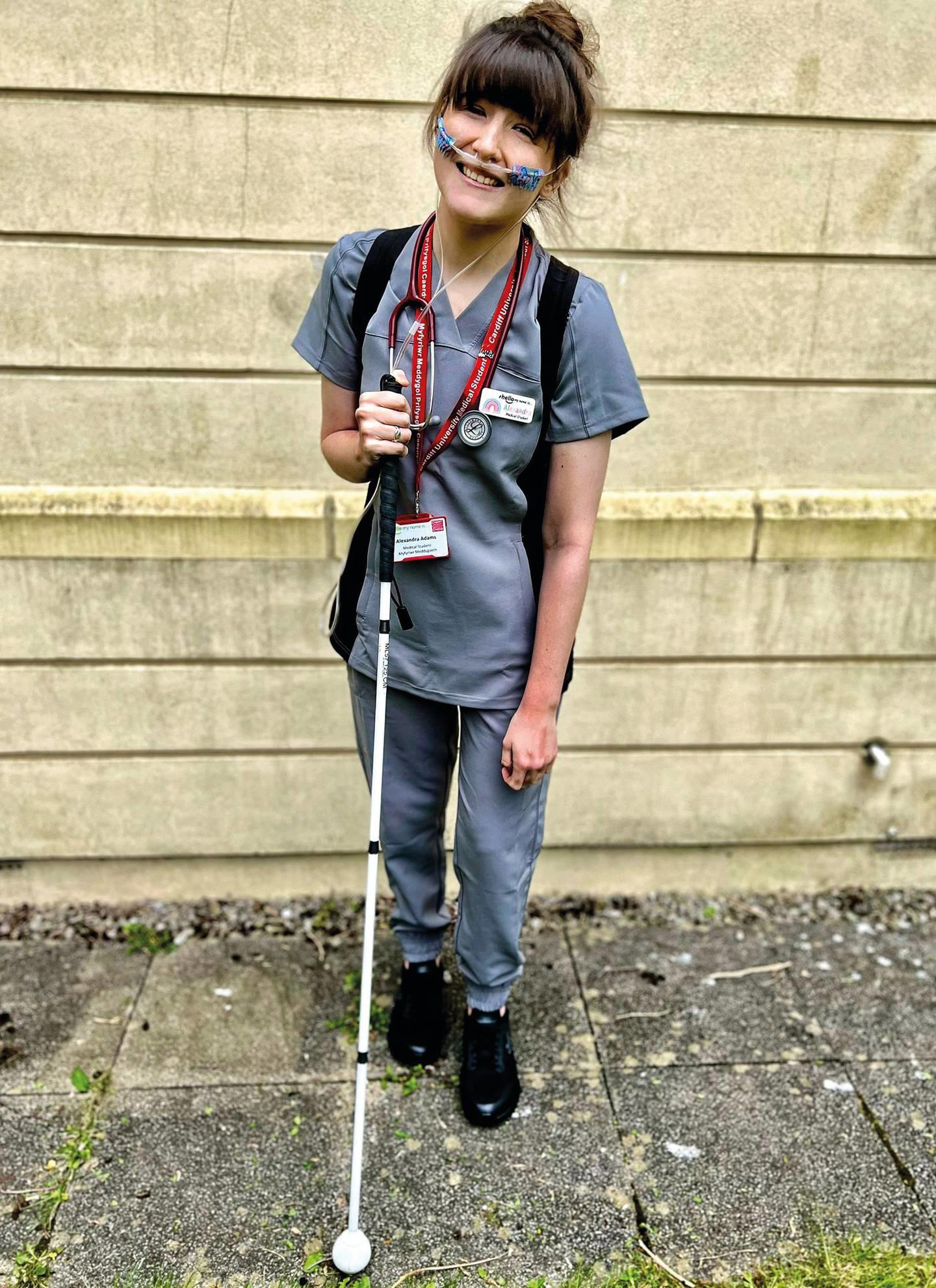
From promoting disability inclusion in sport alongside the likes of Baroness Tanni Grey-Thompson as a teenager, she is now an advocate for diversity in the NHS. Sadly, she has faced discrimination from the public, peers and doctors alike.
Her Faces of the NHS campaign and photo exhibition celebrating diversity in 2019 led to a TEDx talk, and she’s given regular media interviews.
Consistently, it’s her ability to turn tough circumstances to good that has propelled her forward. The year she spent in hospital at 16 inspired her to become a doctor.
This new chapter, marked by chronic illness, has proved far more challenging than her deafblindness. But, if anything, it has made her more determined.
‘I’m not going to lie: there are times when I think: “Oh, stuff it, I hate this,” and you do feel like giving up. But then you remind yourself of the goal and keep going. I’m just trying to focus on the good stuff.’
You can donate to Alexandra’s initiative to buy pianos for hospitals at GoFundMe.

