
‘Life-changing. Devastating. Catastrophic.’ Omer Karim is doing his damnedest to hold back his emotions as he tries to explain the brutal effects a lengthy – and, ultimately, discriminatory – GMC FTP (fitness-to-practise) investigation has had on his existence.
Doctors sometimes speak of the instant, nauseating terror felt when they receive a letter or email with that dreaded three-character heading: GMC. They tell of that stomach-tightening anxiety and panic accompanying a career flashing before their eyes and premonitions of their life crashing down around them.
These are concerns felt even more gravely for doctors from minority ethnic backgrounds – who are more likely to be referred to the GMC by their employer. For Mr Karim, those premonitions were not blown out of proportion. He ‘lost everything’.
Having the investigations hanging over me meant I felt like a prisonerDr Karim
Mr Karim was a consultant urological surgeon at Heatherwood and Wexham Park Hospitals NHS Foundation Trust, (now the Frimley Health NHS Foundation Trust).
During his time there the trust made several investigations into his conduct, eventually referring him to the GMC. After almost four years of investigations, the GMC subjected him to an FTP tribunal. That tribunal was to determine that Mr Karim had done nothing wrong.
 OMER: 'Lost everything' (picture credit: Sarah Turton)
OMER: 'Lost everything' (picture credit: Sarah Turton)
But the process was lengthy and painful. The GMC had first received allegations of concern against him in 2013 and he was officially referred in 2014 but the final FTP hearing – he had been subject to an interim orders process in the meantime – did not take place until April 2018.
In the meantime, Mr Karim lost his private practice and felt forced to leave his trust through a settlement agreement to be able to work elsewhere in the NHS. On top of that Mr Karim sold his family home of 20 years and his daughter left her private school which helped with costs.
Life on hold
Mr Karim, an acknowledged authority in robotic surgery for prostate and kidney cancer, also had to give up teaching roles across the world and was unemployed for five months before taking locum shifts at a south-coast hospital trust miles away from his home, living in a Travelodge when on call.
‘Every family holiday we went on we were constantly wondering whether we would be able to do something like this next year,’ Mr Karim says.
‘We were constantly answering emails from my lawyers and my daughter has lived with this as a huge part of our lives from the age of 15 onwards. Having the investigations hanging over me meant I felt like a prisoner.’
Mr Karim argued that, while the investigations into his conduct continued for years, similar complaints against a white colleague were quickly dropped. In August 2018, he brought claims against the GMC, including a claim of direct race discrimination, and an employment tribunal found in his favour.
In June of this year the tribunal judgment said it was concerned there was ‘a level of complacency about the operation of discrimination in the work of GMC or that there might be discrimination infecting the referral process’.
The judgment also said the GMC was ‘looking for material to support allegations against Mr Karim, rather than fairly assessing matters presented’.
I was mistreated by the very organisation supposed to be looking after meDr Karim
At the FTP hearing in 2018, the GMC failed to disclose evidence which it considered not relevant to the allegations against Mr Karim. Facing prejudice is not a new experience for Mr Karim, who was one of the only minority ethnic boys in a grammar school in the North West.
‘In the NHS it is subtle,’ he says. ‘You applied for jobs and didn’t get shortlisted. If you have a foreign-sounding name you perhaps miss out.’
He adds: ‘In this country, to achieve the same as your white colleagues you have to be better than them. You have to be above everyone just to get the same treatment.’
But experiencing discrimination from his regulator – a body which is supposed to support patients and doctors – was even more galling.
‘I was mistreated by the very organisation supposed to be looking after me, and it was vexing that, the GMC questioned the credibility of their own witnesses,’ he says.
Amazing support
It is not the first time the GMC’s actions have come into question of late.
The BMA is supporting a legal case by the family of Sridharan Suresh, a consultant anaesthetist who took his life within hours of receiving a GMC letter. Dr Suresh’s widow, Viji Suresh, says he was left feeling alone and unsupported.
Mr Karim tells The Doctor he doesn’t think he would have survived his ordeal had he not had such ‘amazing support’ from family, colleagues and friends. Mr Karim’s case has been hailed as a ‘landmark’ moment.
Doctors from minority ethnic backgrounds are already disadvantaged by being referred by their employers to the GMC more than twice as often as their white counterparts – as revealed in the GMC’s own Fair to Refer report, published in 2019.
However, BMA council chair Chaand Nagpaul says the tribunal ruling raises a further ‘significant concern’ that ‘not only do minority ethnic doctors find themselves referred to the GMC more often, but that they can then face further discrimination from [the GMC itself]’.
The judgment said the GMC was “looking for material to support allegations against Mr Karim, rather than fairly assessing matters presented”Dr Nagpaul
Dr Nagpaul says: ‘The profession already feel they are working in exceptionally challenging environments – environments that are unfair for them to work in with too few colleagues, a lack of beds and facilities and capacity nowhere near to meeting demand.
'Our own studies have shown that nine in 10 doctors go into work every day worrying they will make a mistake because of these pressures.
 NAGPAUL: GMC processes must be independently scrutinised
NAGPAUL: GMC processes must be independently scrutinised
‘These pressures are compounded for ethnic minority doctors who suffer twice the level of bullying in the workplace, they feel less confident to speak out about safety concerns due to fear of recrimination or it affecting their careers, on the back of already being disadvantaged with poorer career progression. Many feel isolated and without support from their employer and managers.
'When you add all of that together they are less likely to feel able to challenge or to defend themselves and can become soft targets for blame. The GMC referral is one manifestation of this unequal, unfair existence, and it pervades every area of the system.’
He adds: ‘The GMC has always maintained their [investigations] once the referral has been made are fair but Mr Karim’s case challenges that claim directly. This example will resonate with the views and experiences of so many other ethnic minority doctors who have felt similarly unfairly treated.’
‘Serious misjudgement’
The GMC is appealing the outcome of Mr Karim’s case, arguing that ‘the tribunal wrongly concludes that disproportionate referrals to the GMC by employers constitutes evidence of direct discrimination in Mr Karim’s case’, and also that the case of the doctor with whom Mr Karim was compared differed in key respects.
But doctors from minority ethnic backgrounds told The Doctor they felt the GMC’s refusal to accept the ruling – and to take the opportunity to look at their own processes – ‘crystallised’ worries that the GMC treats doctors from minority ethnic backgrounds differently.
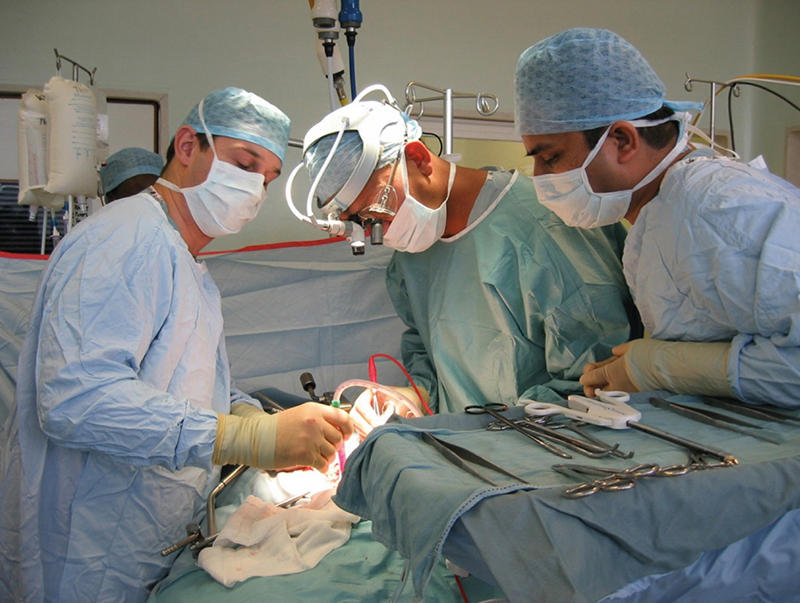 KARIM: Operating, and training other doctors
KARIM: Operating, and training other doctors
Dr Nagpaul says: ‘The GMC should acknowledge there is a desperate need to ensure their own processes are fair and be open about the fact that they may not be. While the GMC also suggests that this is a problem of workplace referrals, we know that GMC employment liaison officers often provide advice on referrals for disciplinary action.
'The right thing – the moral thing – to do is to allow proper, independent, scrutiny of their processes and for the GMC act on any recommendations for change. Given the devastating impact a GMC referral can have on doctors it is imperative that its investigations treat all doctors equally and fairly.’
The BMA is calling for a full, independent, review of the GMC’s FTP processes.

