Update your membership details
In order to properly represent the diversity within the medical workforce and student body, please update your equality data via your member profile when you join or log in. The information you provide is kept strictly confidential and handled in accordance with the GDPR.
The information you provide is kept strictly confidential and handled in accordance with the GDPR.
Stories from the profession
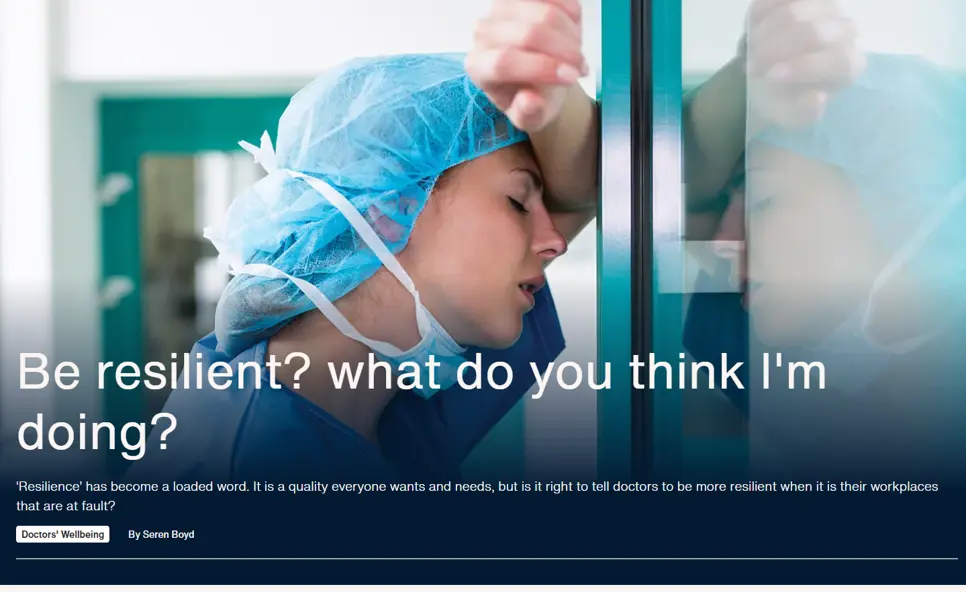
The voice of doctors
Read interviews, investigations and analysis from the BMA on our first dedicated website for The Doctor.
We fight together
Get involved
What members think
 The adviser I spoke to...was fantastic, incredibly well informed and really, really helpful. Your employment advisers are absolutely superb, thank you.Consultant
The adviser I spoke to...was fantastic, incredibly well informed and really, really helpful. Your employment advisers are absolutely superb, thank you.Consultant